The act of brushing and flossing is often relegated to a simple matter of cosmetic maintenance—a routine to prevent cavities and ensure fresh breath. However, a profound and rapidly expanding body of scientific evidence positions oral hygiene not as a standalone practice, but as a critical determinant of overall systemic health. The state of our oral cavity serves as both a mirror reflecting internal well-being and a portal for disease, with poor hygiene being strongly linked to the development and progression of life-threatening conditions, including various cancers, cardiovascular disease, diabetes, and renal failure. This connection, known as the oral-systemic link, transforms the mouth from an isolated ecosystem into a central player in whole-body health.
Periodontitis and the Breach of the Oral Barrier
The primary culprit in this systemic cascade is periodontitis, a severe gum infection that damages the soft tissue and, without treatment, can destroy the bone that supports your teeth. It begins much more innocuously as gingivitis, a reversible inflammation caused by plaque buildup that leads to bleeding gums. When left untreated, the inflammation becomes chronic and the body’s immune response turns destructive.
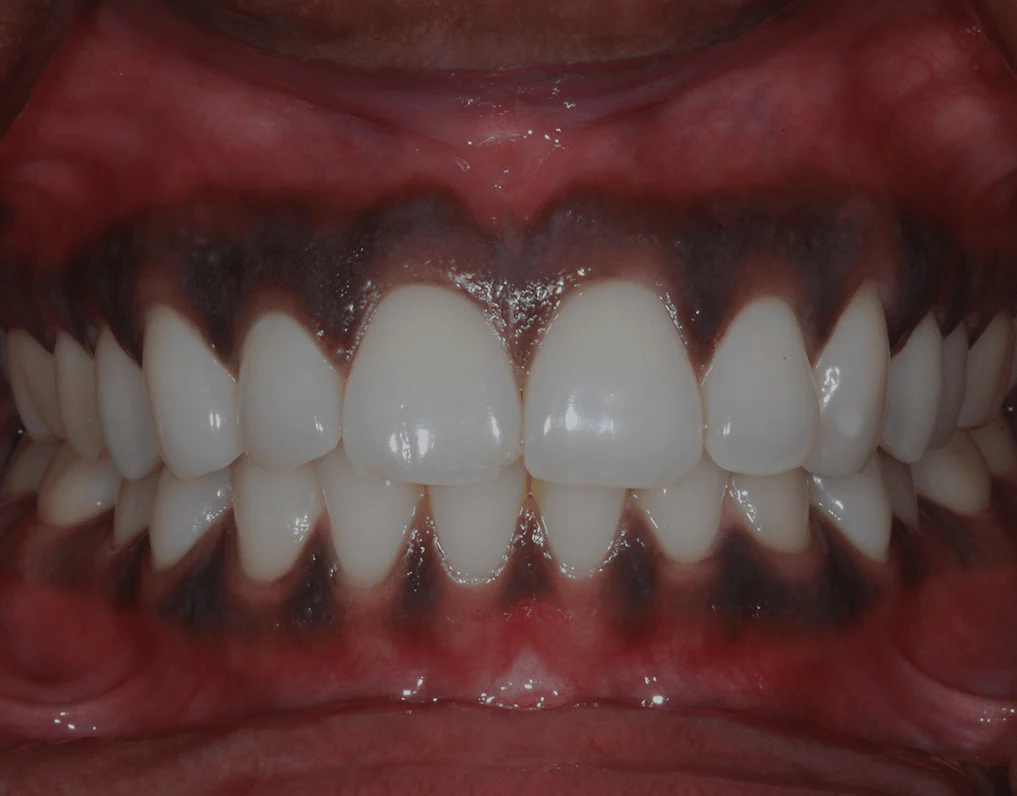
The gums, which should form a tight, protective seal around the teeth, begin to pull away, creating pockets that become infected. This process effectively transforms the vast surface area of the periodontal tissues into an open wound, estimated to be the size of the palm of your hand in severe cases. This breach is the critical event. It allows the estimated 700 different species of bacteria that reside in the oral microbiome—both beneficial and pathogenic—to enter the bloodstream with every chew, brush, or even minor dental procedure. This constant seeding of bacteria into the circulation, a condition known as bacteremia, and the accompanying release of inflammatory mediators, is the engine that drives systemic disease.
The Cancer Link: Bacterial Drivers of Malignancy
The connection between oral pathogens and cancer is one of the most alarming and actively researched areas. A pivotal 2018 study published in The Lancet Oncology provided robust epidemiological evidence, analyzing data from thousands of participants and finding a significantly elevated risk of pancreatic and gastrointestinal cancers in individuals with a history of gum disease and tooth loss.
The mechanism extends far beyond general inflammation. Specific pathogens have been identified as direct actors in carcinogenesis. Fusobacterium nucleatum, a common bacterium in dental plaque, has been found in abnormally high levels in colorectal cancer tumors. Researchers like Dr. Dominique Michaud, a cancer epidemiologist at Tufts University, explain that this bacterium is not a passive bystander. “Oral pathogens like Fusobacterium nucleatum don’t stay confined to the mouth—they travel through the bloodstream and to distant sites,” she states. Once there, they employ sophisticated strategies to promote tumor development: they can suppress the local immune system’s ability to recognize and attack cancer cells, they create a pro-inflammatory environment that encourages cellular damage and rapid growth, and they may even directly help cancer cells survive and metastasize. Furthermore, the body’s chronic inflammatory response to these bacteria generates free radicals and enzymes that can cause DNA damage in otherwise healthy cells, initiating the cancerous process.
The Heart of the Matter: Inflammation, Atherosclerosis, and Endocarditis
The American Heart Association has consistently identified periodontitis as an independent risk factor for cardiovascular diseases, including heart attacks and strokes. The pathway is primarily through the acceleration of atherosclerosis—the hardening and narrowing of arteries due to plaque buildup.
The bacteria entering the bloodstream from the infected gums, particularly Porphyromonas gingivalis and Streptococcus sanguinis, adhere to fatty plaques already present in the arterial walls. The body’s immune system, recognizing these invaders, launches a fierce attack, causing chronic inflammation within the blood vessel itself. This inflammatory process makes the existing plaque unstable and more likely to rupture. A ruptured plaque can form a clot that blocks blood flow to the heart (causing a myocardial infarction) or to the brain (causing an ischemic stroke). Furthermore, the systemic inflammation caused by the oral infection leads to the liver producing elevated levels of C-reactive protein (CRP), a key marker of inflammation that is also directly implicated in cardiovascular risk. For individuals with pre-existing heart valve conditions, these circulating oral bacteria can also attach to the damaged valves, causing a dangerous and often fatal infection known as infective endocarditis.
Beyond the Heart: Renal Decline, Diabetes, and Respiratory Complications
The repercussions of oral inflammation extend to other vital organ systems. A 2020 study from the University of Birmingham analyzed the health records of over 100,000 patients and found that those with periodontitis had a twofold higher risk of progression to end-stage chronic kidney disease (CKD). The constantly overworked immune system and chronic inflammation put immense strain on the kidneys, whose function is to filter waste from the blood. This inflammatory state accelerates the scarring (fibrosis) and degradation of renal tissues.
The relationship with diabetes is particularly bidirectional. Periodontitis makes it more difficult for diabetics to control their blood sugar levels. The systemic inflammation increases insulin resistance, creating a vicious cycle where high blood sugar also promotes gum disease by impairing white blood cell function and healing. Furthermore, the aspiration of oral bacteria into the lungs can lead to respiratory infections like pneumonia, especially in elderly or hospitalized patients, by introducing pathogenic colonies directly into the respiratory tract.
A Call for a Paradigm Shift in Healthcare
The evidence mandates a fundamental shift in how we perceive dental care. “Your oral health is a window into your overall health,” says Dr. Michael Glick, Professor of Oral Diagnostic Sciences. “Ignoring your teeth isn’t just about risking a cavity; it’s about quietly permitting a constant source of inflammation and infection that can damage vital organs over a lifetime.”
This understanding bridges the historic divide between medical and dental care. It argues for the integration of oral health assessments into routine physical examinations and for greater collaboration between physicians and dentists. For the public, the message is clear: consistent oral hygiene—brushing twice daily with fluoride toothpaste, daily flossing to disrupt biofilm between teeth, and regular professional cleanings—is no longer just about preserving a smile. It is a non-negotiable, proactive investment in long-term systemic health, a powerful and accessible form of disease prevention that truly has the potential to save lives.





